Attention
This website serves the purpose of providing general information and does not in any way replace medical or specialist advice. Consult a healthcare practitioner if symptoms worsen or persist.
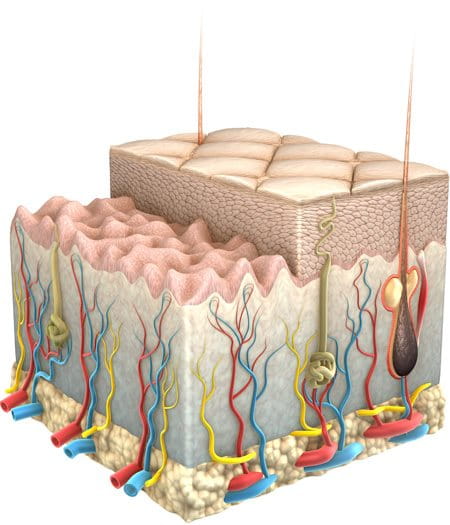
Young skin looks and functions differently to adult skin. The self-protection mechanisms prevalent in healthy adult skin are less developed and, as a result, babies and children need special care to keep their skin feeling and looking healthy.